Plantar Fasciitis
Plantar Fasciitis is a common cause of heel and foot pain resulting from inflammation and degeneration of the connective tissue at the underside of the foot.
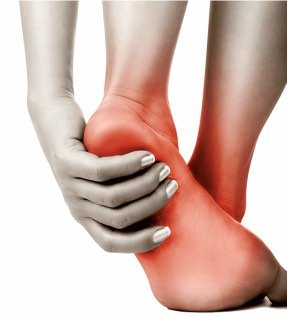
Plantar Fasciitis Explained
The plantar fascia is a strong band of connective tissue that runs along the sole from the heel to the ball of the foot. It supports the arch of the foot and keeps the bones and joints in position. It also creates a spring-like effect which absorbs shock and enables you to push off from the ground when walking.
Fascia can undergo a degenerative process called fasciopathy. Over time, the normal elastic collagen fibres become weaker and less elastic. This results in overstretching and tearing of the fascia itself, resulting in inflammation and pain on the underside of the heel.
Plantar fasciitis can also be associated with a heel spur which may also contribute to your heel pain.
Signs and symptoms
Pain is usually felt on the inside part of the bottom of the heel. The area can be very tender and swollen and it may feel like a stabbing pain in the bottom of the foot when weight bearing. People often say it feels like they have stood on a stone and bruised the heel.
Pain from plantar fasciitis can begin after a walk, run or standing on a hard surface for extended periods. Sometimes a person cannot relate the pain to any obvious cause or incident.
The pain is usually most intense with the first steps of the day or after prolonged sitting or rest. Prolonged periods of standing, climbing stairs, exercising, and standing on tip toes can all aggravate the pain of plantar fasciitis.
Risk factors for Plantar Fasciitis
- Sports or activities that place a lot of stress on the heel and feet - like running, dancing and aerobics.
- Flat feet or high arches. People with flat feet may have reduced shock absorption which increases strain on the plantar fascia. High-arched feet have a tighter plantar tissue, leading to similar effects.
- Muscles supporting the arch of the foot can become weaker with age, thereby putting stress on the plantar fascia.
- Being overweight places a greater mechanical load on the plantar fascia. There is evidence that overweight and inactivity lead to chemical damage to the plantar fascia.
- Weight gain, swelling and hormonal changes that accompany pregnancy may lead to a mechanical overload of the plantar fascia.
- Being on your feet for prolonged periods. Occupations that require a lot of walking or standing on hard surfaces may predispose you to plantar fascia pain.
- Worn or poorly designed shoes with bad arch support or stiff soles.
- Tight calf muscles can affect normal foot biomechanics, thereby placing more strain on the plantar fascia
- Trigger points in the lower leg and foot muscles can cause pain in the heel
Other Pain You Might Feel
Heel Pain
Are you feeling pain in your heel? Find out what might be the cause and how we can help.
How do we treat plantar fasciitis?
In any type of muscle or joint problem, the first step is to get an accurate history which enables us to understand your general health, past-history, and lifestyle. We then perform a thorough assessment of your feet, lower limbs and spine. We look at the health and condition of the muscles, joints and tendons in your feet, legs and spine. Importantly, how your feet and legs function during walking and standing can play an important part in the development of plantar fasciitis and foot pain of all types.
Once we have a clear diagnosis and understanding of your foot problem, we outline and discuss a treatment program which often includes:
- Stretching of the foot and leg muscles and plantar fascia
- Soft tissue therapy to release tight muscles in the legs and feet. This may include trigger point therapy, myofascial release and lymphatic drainage.
- Cold Laser to relieve pain and promote healing
- Taping to support the plantar fascia while it heals
- Manipulation of the joints of the feet and lower limbs
- Prescription of arch supports or orthotics to assist normal foot function
Referral to our podiatrist for specialised assessment of the biomechanics of your feet is important to ensure quick recovery and prevention of future problems. Our podiatrist will advise you on proper foot wear and the possible need for orthotics or arch supports to improve and support foot function.
Active Care is very important and includes stretching and strengthening exercises to improve the health and function of the muscles, ligaments, tendons and fascia in the feet and legs. We will advise you how to self-manage your recovery and how to strengthen your legs and feet to ensure a healthy and pain-free future.
A summary of our goals during your treatment program
- Identify and correct biomechanical dysfunction.
- Decrease pain and inflammation.
- Improve flexibility and strength of the plantar fascia.
- Return to full fitness.
- Prevent future problems and possible re-injury.
At Burswood Health, our team of chiropractors, soft tissue occupational therapists and podiatrists will work together to treat your plantar fasciitis in a manner that relieves pain and prevents future problems. The first step is to contact us to arrange an appointment. Our friendly staff are here to help answer all of your questions.